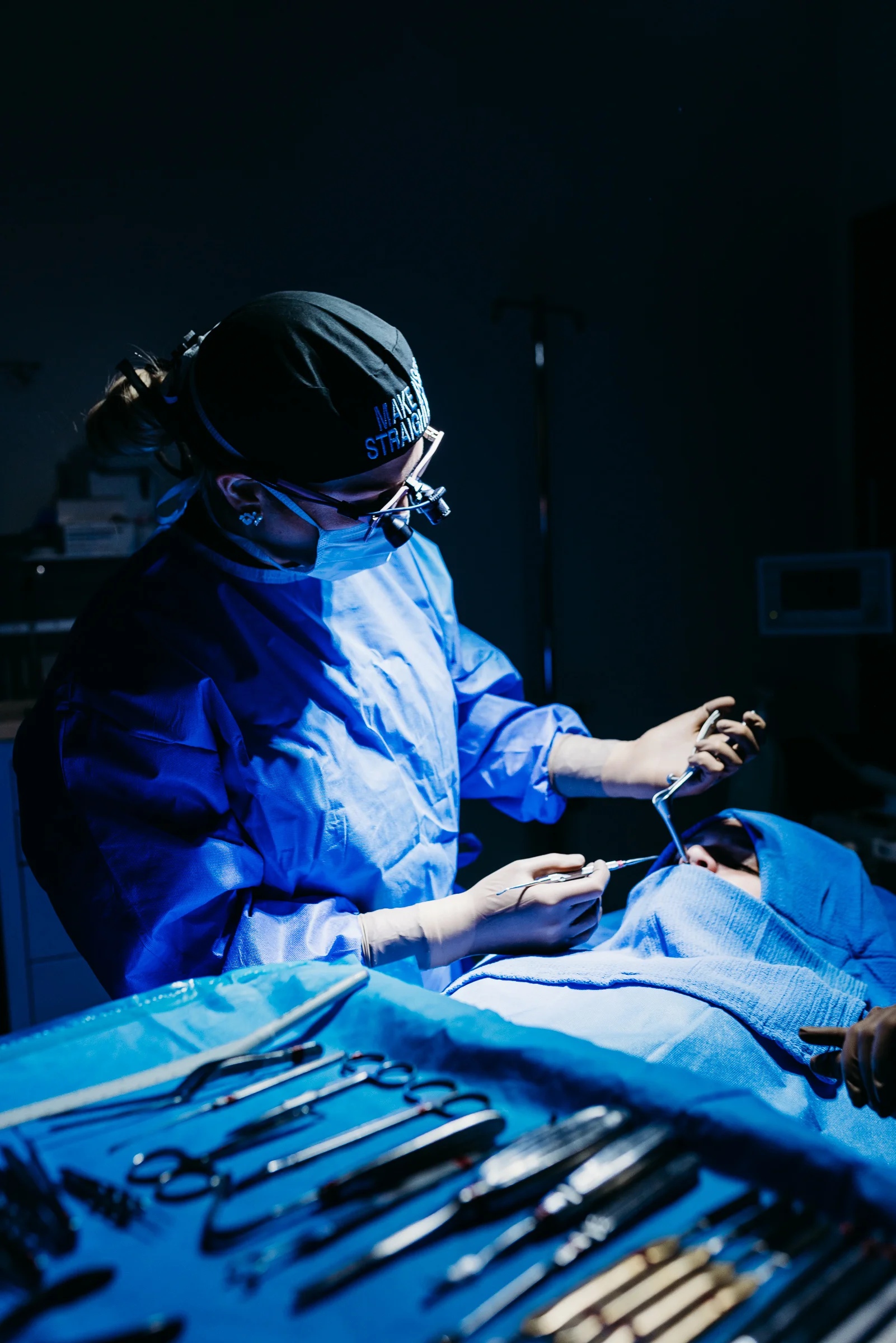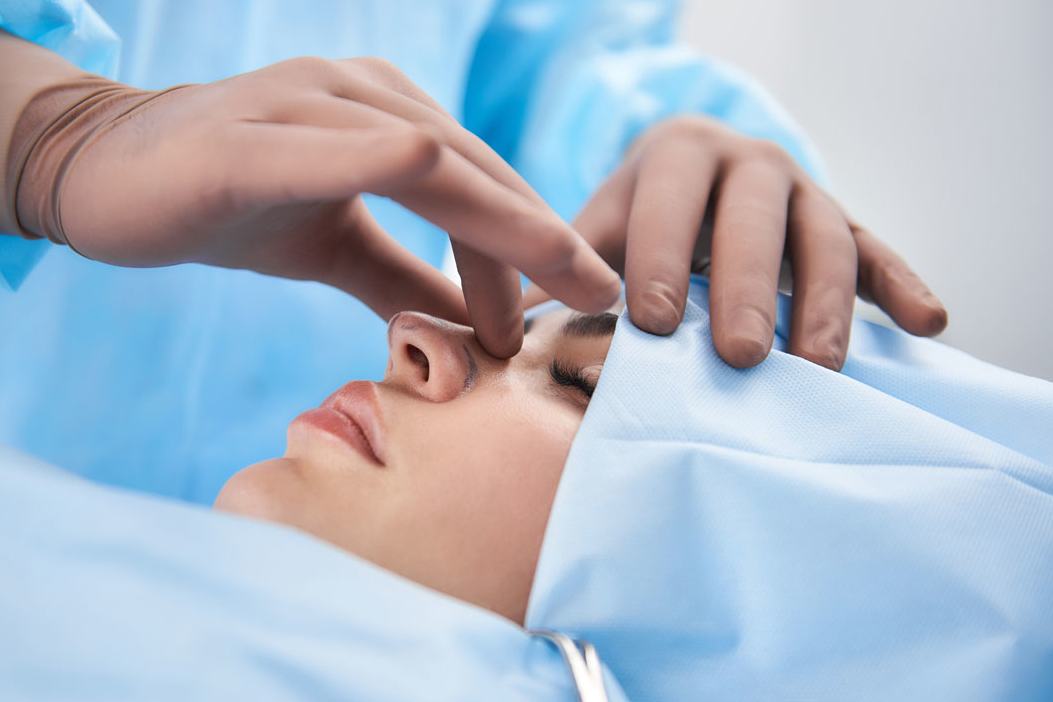
NSIBR |Featured, Procedures, Rhinoplasty | October 5, 2020
Our practice focuses on the inside and outside of the nose. Patients come to us to alter the appearance of the nose, to help with their functional issues, or a combination of the two. Patients who have had previous rhinoplasty surgery and have issues regarding that procedure, whether the original issue wasn’t totally corrected, maybe it was made worse, or sometimes maybe it is an issue that arose from that procedure, present a unique and usually frustrated group. They require extensive evaluation and analysis. These patients are often very reluctant to undergo a second (or more) nasal procedure after their results from the original procedure were less than satisfactory. The following are the commonly asked questions and how we attempt to answer them.
Why do I need more surgery on my nose?
This question is almost universal and reflects the frustration that many patients have that have gone through a prior rhinoplasty (or rhinoplasties) and are faced with needing an additional surgery. There are many reasons for needing additional surgery. They can be broadly categorized as cosmetic issues and functional issues.
Some patients noticed these issues from the time the original surgery was performed. Others will come to the office having had a satisfactory result from their original surgery but a gradual issue which subsequently. Cosmetically this typically is caused by shrinking of the skin envelope of the nose causing telltale signs of the previous rhinoplasty: an overly narrowed tip, retraction of the tip, collapse of the tip, rounding of the tip, irregularities of the bridge of the nose, or other unsightly signs of the previous surgery. Functionally, many patients complain of progressive nasal obstruction, This also may be secondary to many factors (see question 2 below), most frequently to a slowly progressive collapse of the integrity of the lateral walls of the nose. Immediate functional impairment following rhinoplasty can also be due to inadequate strength of the remaining framework or persistent deviation of the nasal septum.
Rhinoplasty is an art and depends not only on the surgeon’s skill and experience, but also on optimal healing. If too much of the structural framework of the nose has been removed and not rebuilt, then over time the skin of the nose can ‘shrink wrap’ around the remaining framework and cause both cosmetic and functional issues.
Any of these problems may necessitate further surgery. The exact nature and extent of the surgery will directly depend upon the complexity of the underlying issue.
Why can’t I breathe?
When a patient comes in for a consult stating that following their rhinoplasty they noticed immediately that they no longer could get adequate airflow through their nose, it is most often from an anatomic issue resulting from the rhinoplasty. If too much of the framework has been removed during the initial rhinoplasty then the walls of the nose will weaken. Patients with this issue will often state that they can manually pull their cheeks towards their ears and get improved airflow. This is known as a ‘Cottle sign’. In analyzing this issue, we will place a cotton tip applicator or a curette inside the nose to stabilize the lateral wall of the nose and ask if that alleviates the breathing issue. If it does, then that indicates a weakened lateral wall is causing the nasal valve to collapse. Another issue frequently encountered is a persistent deviation of the nasal septum. This is diagnosed by exam including a nasal endoscopy.
Some patients state that they were having breathing issues prior to rhinoplasty surgery and that following the surgery their issues were either not improved or were made worse. In addition to the lateral nasal wall and nasal septum problems discussed above, we also consider previously undiagnosed blockage caused by turbinate hypertrophy or sinus disease. These are diagnosed by history, exam, nasal endoscopy, and possibly a CAT scan of the nose and sinuses. If the obstruction is solely due to turbinate hypertrophy (typically from allergies), then it may respond to a steroid nasal spray and allergy control. If there is sinus blockage diagnosed, then medical management and perhaps a balloon sinuplasty may be recommended. Once the surgeon has determined the cause of the breathing problem, he can offer the best and most conservative plan to pursue.
Can my sinus issues be handled at the same time as my revision rhinoplasty surgery?
Yes, and it makes good sense to take care of the ‘total nose’ at one sitting. The ‘total nose approach’ became possible after minimally invasive procedures were developed for the sinuses in the 1980s. These procedures, introduced in the United States at the Johns Hopkins Hospital, enabled surgeons for the first time to fix the outflow track of blocked sinuses through a telescope. This immediately changed the sinus surgery experience to a minimal downtime outpatient procedure. Balloon sinuplasty has taken the concept of ‘minimally invasive’ to an even more delicate level. These procedures are now performed in the doctor’s office when done as stand alone procedures. When combined with rhinoplasty or revision rhinoplasty, they are performed either in the office or an outpatient surgical facility.
How long should the surgery take?
Depending upon the extent of the issue(s), revision rhinoplasty can take anywhere from 30 minutes to five or six hours. Whether the original surgeon used an open rhinoplasty (incision along the bottom of the nose) or closed rhinoplasty (no external incision) technique, revision rhinoplasties are mostly done through an open technique. This is especially true if restoration of the framework of the nose is required. This rebuilding of the framework of the nose requires good exposure and longer operative time. Suturing these grafts in place is a meticulous and labor intensive process.
Why is revision rhinoplasty so much more expensive than my first surgery? Will insurance cover any of the expense?
It is not uncommon for revision rhinoplasty to be two to three times as expensive as the original rhinoplasty. This is mostly due to the amount of time it takes to perform. A primary rhinoplasty depending upon the issues being treated and the approach (closed vs. open) can take as little as one to two hours. Open revision rhinoplasty can require five to six hours. This increase in time spent is reflected not only in the surgical price, but also the facility and anesthesia fees. Depending upon coexisting functional issues, some of the expense may be covered by a patient’s insurance company. The surgeon’s staff will assist the patient in this determination.
How long will the recovery be?
Most patients return to work or school within five to seven days of surgery. This timing coincides with removal of the external splint. If the bones need to be repositioned during the revision rhinoplasty, then there may be some bruising beneath the eyes. Otherwise bruising is usually not present or is minimal. Typically there is little nasal pain following this procedure and in our Institute packing is not used. There might be minor discomfort if cartilage is taken from behind the ear and minor to moderate discomfort if a piece of rib cartilage is required. In certain situations patients may prefer using rib cartilage from a tissue bank rather than their own tissue. That is a discussion based on patient and surgeon preference and will be done during the consultation.
Who would be the best surgeon to perform my revision rhinoplasty?
The best surgeon to perform revision rhinoplasty is one whose practice concentrates on these procedures. It is a specialty in and of itself. The right surgeon is best determined by communication between the patient and the surgeon during the consultation, reviews of other patients who may have had similar experiences, physician referrals, and friend and family referrals. Before and after photos may help, but reviews tend to cover the whole gamut of issues and experiences.
The Nose and Sinus Institute of Boca Raton has been caring for patients in Florida and surrounding regions for over three decades. Drs Nachlas and Hancock specialize in medical, allergic, and surgical care of the nose, sinuses and face. Both surgeons are double board certified – otolaryngology as well as facial plastic surgery. Many state of the art procedures for the minimally invasive treatment of these areas were pioneered at the NSIBR, including minimally invasive sinus surgery, in office computer assisted balloon sinuplasty (first in the United States, performed in 2014 at NSIBR), balloon septoplasty and noninvasive sculpting of the nose for breathing relief. Patients undergoing any or all of these procedures at the Institute can elect to have these performed under local anesthesia or under light anesthesia. For more information, please contact Sandy Friedman, our Director of Patient Relations, at 561-939-0909.